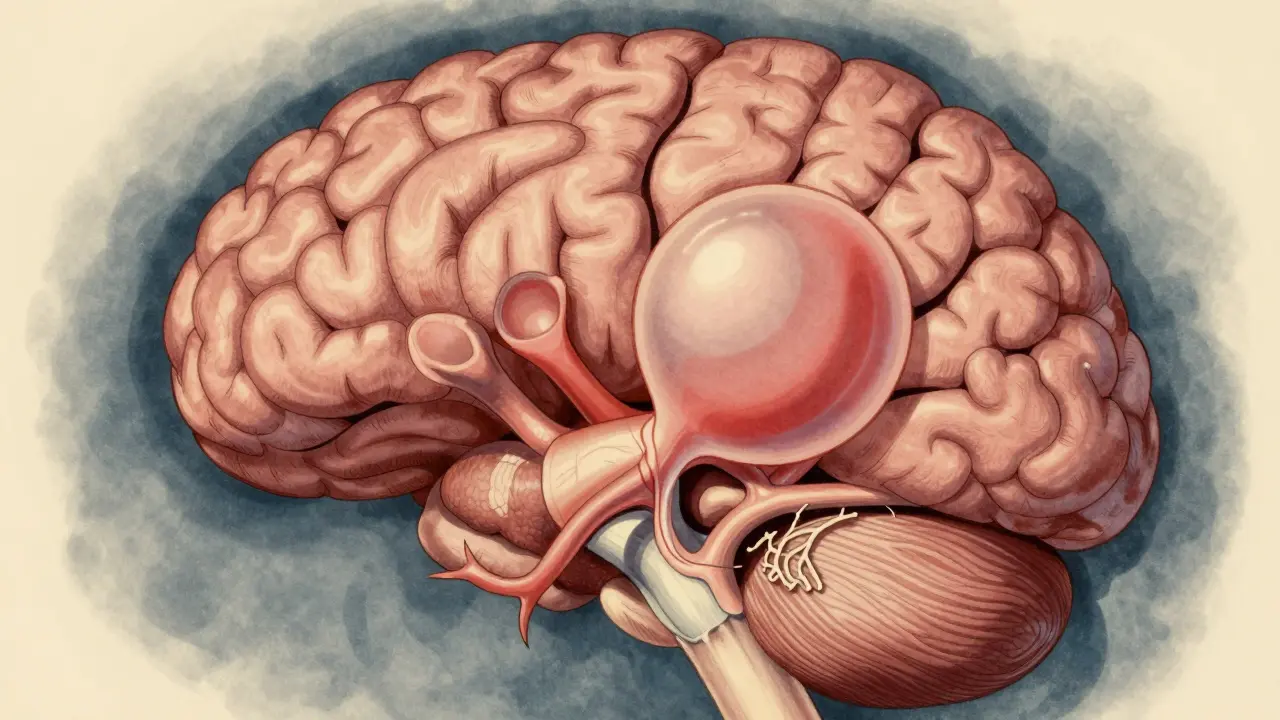
Cerebral Aneurysm is a pathological dilation of a cerebral artery where the vessel wall weakens, forming a sac-like protrusion that carries significant risk of rupture leading to subarachnoid hemorrhage. Also known as brain aneurysm, it affects approximately 3.2% of the global population. While most remain silent, the danger lies in potential rupture. When this balloon-like bulge bursts, it causes bleeding inside the skull known as subarachnoid hemorrhage. Recent data from 2024 indicates that roughly 9 to 10 people out of 100,000 experience this annually. The stakes are incredibly high; mortality rates hover around 30-40% within the first day of a rupture. That is why understanding the warning signs and risk profiles is critical for anyone concerned about their brain health.
The Mechanics of Rupture Risk
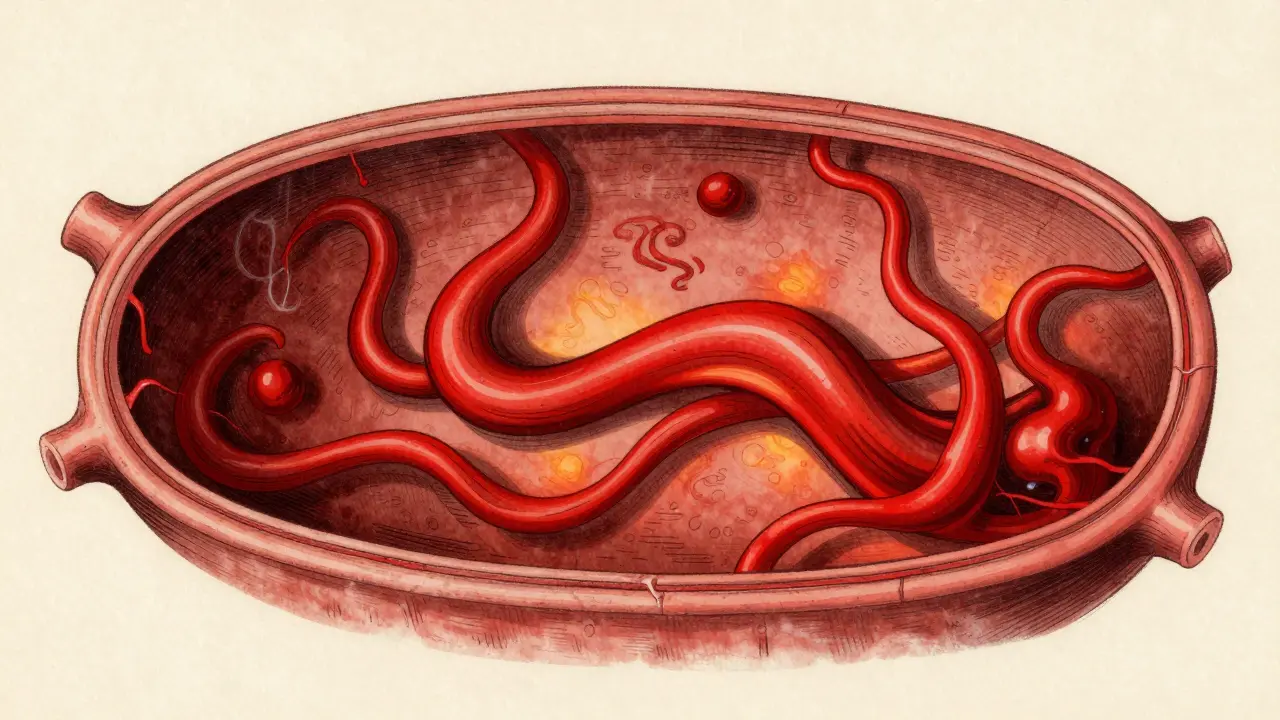
Not every bulge leads to disaster, but predicting which ones might fail requires looking at specific details. Doctors evaluate morphology, or shape and size. If an aneurysm measures 7 millimeters or larger, the hazard ratio for rupture jumps significantly compared to smaller ones. Irregular shapes carry even more weight than size alone. Specifically, those with daughter sacs-small lobes growing off the main pouch-have a 68% higher risk compared to smooth, spherical ones. Location matters immensely too. Aneurysms on the middle cerebral artery show higher instability, while those on the anterior communicating artery (AComm) often rupture despite being smaller.
Beyond anatomy, biology plays a huge role. Inflammation markers like CRP and IL-6 are often elevated in patients who suffer a rupture. These biological signals suggest that the vessel wall is under stress long before the physical break happens. Hemodynamic forces, essentially the way blood flows and presses against the walls, also dictate stability. Low and oscillatory wall shear stress correlates with rupture in the vast majority of cases. This means turbulent blood flow weakens the vessel over time. Understanding these mechanics helps explain why some patients with similar-sized aneurysms have vastly different outcomes.
Identifying Your Personal Risk Factors
Risk isn't just about luck; it's about your lifestyle and genetics. You cannot change your age, but statistics show individuals over 65 face a 2.7-fold increase in rupture risk. Gender is another factor, with women having a 1.6-fold higher prevalence than men. Genetics run deep here as well. If two or more first-degree relatives have had a brain aneurysm, your personal risk increases four-fold. However, the factors you can control offer a powerful buffer against catastrophe.
Hypertension is arguably the biggest controllable enemy. Maintaining systolic blood pressure above 140 mmHg increases rupture likelihood by 2.3 times. Chronic tobacco use is another major culprit. Current smokers face a 3.1-fold higher risk compared to non-smokers. Interestingly, the relationship is dose-dependent, meaning smoking more cigarettes daily compounds the damage. Even alcohol consumption plays a part; exceeding 14 drinks weekly raises risk by 32%. By managing these variables, you directly lower the probability of a bleed.
Prediction Models: PHASES and Beyond
Doctors do not guess when deciding whether to intervene. They rely on validated scoring systems. The most prominent tool is the PHASES score. This model combines six factors: Population, Hypertension, Age, Size, Earlier Subarachnoid Hemorrhage, and Site. It predicts the 5-year rupture risk accurately. A score of 0-3 points suggests a low annual risk of around 3%, while scores hitting 9-10 points indicate a grim 45% risk over five years. Another useful metric is the ELAPSS score, which refines this further to estimate 1-year probabilities. For patients worried about growth rather than immediate rupture, the triple-S model looks at size, site, and shape to forecast expansion.
These numbers guide clinical decisions. A patient with a small aneurysm in a stable area might get a green light for monitoring. Conversely, someone with a high PHASES score usually qualifies for intervention. Patients with multiple aneurysms face a complex scenario; they see a 3.8-fold higher rupture risk than those with solitary lesions. Previous history of rupture also skyrockets danger, increasing subsequent rupture risk by more than 5-fold. Using these mathematical models ensures treatment matches actual danger levels.
Treatment Options: Surgery vs. Interventional Radiology
When intervention is necessary, there are generally three main paths available today. The choice depends on aneurysm characteristics and the patient's overall health.
Procedure
Success Rate (Occlusion)
Re-treatment Need
Invasiveness
Surgical Clipping
95%
Low (6.2%)
High (Craniotomy)
Endovascular Coiling
78-85%
Moderate (15.7%)
Low (Catheter-based)
Flow Diversion
76.4%
Variable
Moderate (Stent)
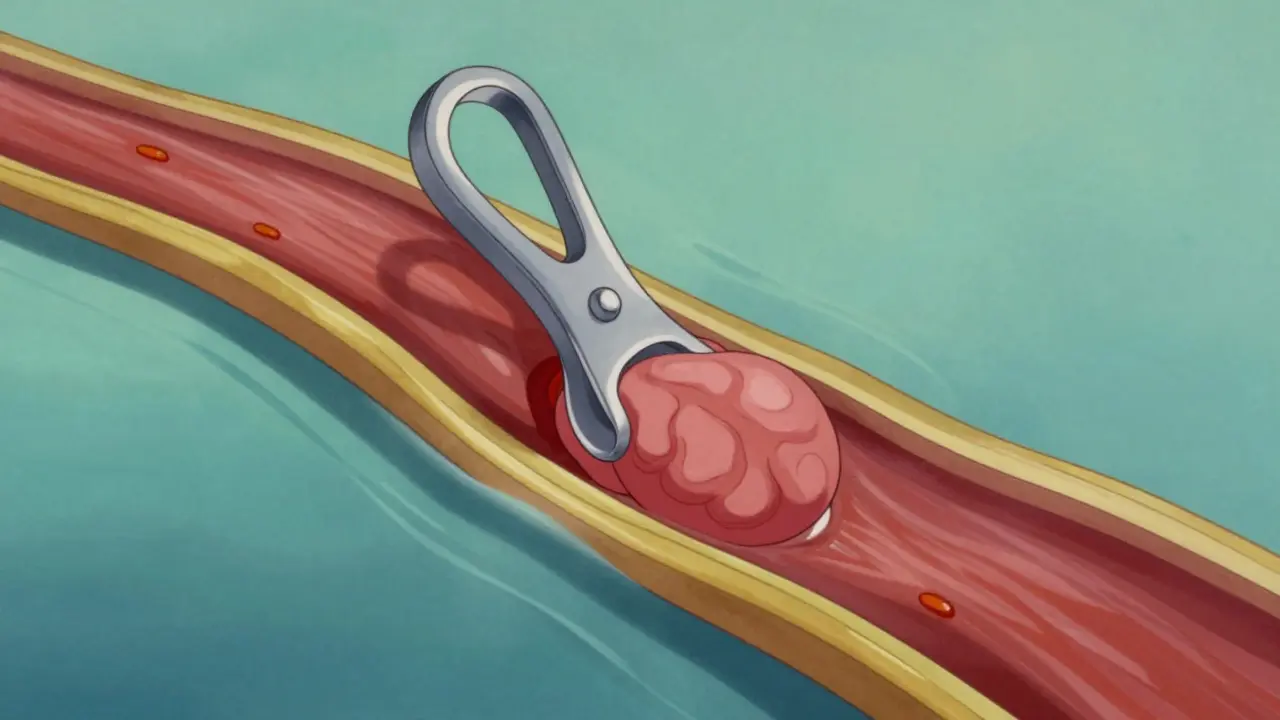
Surgical Clipping is a method pioneered in 1937 involving craniotomy to place a titanium clip across the aneurysm neck, achieving complete occlusion in 95% of cases. This open surgery permanently isolates the bulge from blood circulation. It offers a high permanent cure rate, sitting between 88-92%. However, because it involves opening the skull, complications are slightly higher. Patients over 70 face a 35% increase in surgical complication rates, making this option less favorable for the elderly.
Endovascular Coiling is a minimally invasive procedure using catheter-based delivery of platinum coils to induce thrombosis within the aneurysm sac. First performed in 1991, this technique reduced 1-year mortality compared to clipping in major trials. It accesses the vessel through arteries in the groin. The trade-off is durability. Retreatment rates are higher, meaning you might need follow-up procedures to ensure the coil mass stays intact. Success rates hover around 85% complete occlusion at six months.
For large or wide-necked aneurysms, a newer technology called Flow Diversion is now standard. This uses porous stents to redirect blood flow away from the weak spot, allowing the body to seal it naturally. Devices like the Pipeline Embolization Device achieved FDA approval around 2011. They show high success for giant aneurysms but require antiplatelet medication post-procedure, which adds its own risks.
Lifestyle Management and Prevention
Even after diagnosis, daily habits drive long-term safety. Medical management focuses intensely on strict blood pressure control, targeting readings under 130/80 mmHg. Quitting smoking provides a rapid benefit; stopping reduces rupture risk by 54% within two years. Alcohol moderation is also recommended, keeping intake within safe limits. For unruptured aneurysms, many experts support conservative management if the size is under 5mm, especially in posterior circulation. Studies like UCAS Japan found a 5-year rupture risk of merely 0.7% for tiny aneurysms in specific locations, supporting watch-and-wait strategies.
What Happens After Treatment?
Successful treatment drastically improves the outlook. Once secured, the 10-year re-rupture risk drops from 68% down to 2.3%. Quality of life measurements consistently show better scores for endovascular approaches compared to open surgery in the first year. However, vigilance remains key. Follow-up imaging is mandatory. Annual MRA scans are typically advised for monitored cases to catch any growth early. Complication rates vary, but morbidity for coiling sits around 3.9% and mortality at 1.1% according to 2023 guidelines. Understanding these figures helps you weigh benefits against risks realistically.
Can a cerebral aneurysm heal on its own?
Generally, no. The weakness in the vessel wall does not reverse itself spontaneously. However, if an aneurysm has already ruptured, the body may form a clot that temporarily seals the leak, but this does not guarantee safety or prevent re-bleeding.
What are the immediate symptoms of a rupture?
The hallmark sign is a sudden, severe headache often described as a "thunderclap." Other symptoms include vision problems, nausea, stiff neck, and loss of consciousness. Immediate medical attention is vital as mortality is highest in the first 24 hours.
Is surgery always required for an aneurysm?
Not always. Small aneurysms in low-risk locations often fall into the "monitoring" category. Guidelines from 2023 suggest observation for sizes under 7mm without irregular shape or high-risk features.
How often should I monitor a small aneurysm?
Typically, neurosurgeons recommend annual Magnetic Resonance Angiography (MRA) scans to track stability. If growth is detected, the protocol shifts immediately toward considering intervention.
Does family history guarantee I will develop one?
It significantly increases risk, specifically if two first-degree relatives are affected. Screening via MRI is strongly recommended for these individuals, even if asymptomatic, to catch issues before they grow dangerous.






Paul Vanderheiden
glad you shared this stuff really scary how many people have them but good news we can treat it now so stay positive everyone
keep checking your health friends matter too
kendra 0712
This is incredibly informative!!! I appreciate the breakdown of the PHASES score!!! It is so important to know your family history!!! My mom had one and the screening saved her life eventually!!!
tyler lamarre
Sure lets panic about blood vessel balloons instead of actual things that kill people immediately like obesity or car accidents obviously statistics matter but do we really need a table for clip success rates who reads tables anyway
Tony Yorke
Good read on the flow diversion tech though surgery looks intense for sure.
Rohan Kumar
lol tyler is scared 😂👌 the big pharma wants us clipping heads open💊 they dont mention herbs that heal walls naturally 🤡 why trust doctors anyway 🙄
Richard Kubíček
Life is full of uncertainties sometimes the body fails us unexpectedly knowing the mechanics helps prepare us mentally even if the risk is low statistically most live normal lives despite the potential threat looming in shadows
Monique Ball
Oh my gosh that conspiracy theory comment is totally wild! 🙅♀️ You really need to understand that science takes years to validate claims like herbal cures for vascular issues! ⚠️ I have spent countless hours researching neurology papers to help patients feel safer during diagnosis! 😅 Ignoring blood pressure management is actually really dangerous for aneurysm growth! 📉 Every study confirms hypertension doubles the risk factors significantly without fail! 👩⚕️ Smoking cessation alone drops the risk by half which is amazing progress possible today! 🚭 Doctors aren trying to hide natural remedies but they simply cant work magic on torn arteries instantly! ✋ It is crucial we follow guidelines from the 2023 updates regarding MRA scans for monitoring small ones! 💻 Please listen to certified experts when discussing rupture prevention strategies carefully! 📝 We want everyone staying healthy and informed about their own specific biological markers daily! ❤️ Do not gamble with your brain health over unverified internet anecdotes please! 🧠 Regular checkups save lives every single day across the globe consistently! ✅ Trust modern medicine for something as serious as subarachnoid hemorrhage cases rising globally! 🌍 Staying vigilant makes all the difference in managing long term safety outcomes well! 🛡️ Many families benefit from knowing these statistical probabilities clearly!
Austin Oguche
In my country we see high hypertension rates making this data vital for public health education efforts broadly speaking
Sarah Klingenberg
Yeah lifestyle differences definitely play huge roles here :) genetics aside managing stress helps everyone stay balanced and safe
Shawn Sauve
Thanks for sharing the clear info on rupture risks and warning signs 🙂 hope this helps someone recognize symptoms early
walker texaxsranger
hemodynamic shear stress values ignore endothelial nitric oxide synthase regulation entirely just like coiled embolization fails long term patency rates in posterior circulation aneurysms fundamentally flawed paradigm
Eva Maes
Typical doom scrolling content designed to frighten laypeople into unnecessary interventions ignoring quality of life metrics entirely while surgeons profit massively from craniotomy procedures nobody discusses adequately